Brought Back From the Brink
A practical and theological reflection on how Naloxone, the ‘Lazarus Drug’, is saving lives
The still body lay crumpled in the dawn light at the bottom of the steps to Blackpool Salvation Army’s Bridge Project, a church-based homeless day centre. As staff arrived at work, they saw the distressing scene in the form of a woman, awkwardly sprawled, leaning against cold brickwork and unforgiving concrete stairs. Approaching the body, Jill, the steadfast manager of the project, could see some slight movement. The urgency became palpable as she took command. The staff kicked into action.
“Quick - get the naloxone! And call an ambulance!”
It was Beth. Her limp yet living body was showing signs of overdose: loss of consciousness, unresponsiveness, shallow breathing, and lips and fingers turning a lavender blue hue. Time left no room for hesitation. A colleague returned. He placed the naloxone in Jill’s hands. With calm resolve, she administered the pre-filled syringe into Beth’s thigh.
Beth woke.
The ambulance arrived. The paramedics took Beth to the hospital. Jill and the team, having averted a crisis, retreated inside for a brew. The moment of respite with a cup of tea gave them time to prepare to face whatever else the day might throw at them.
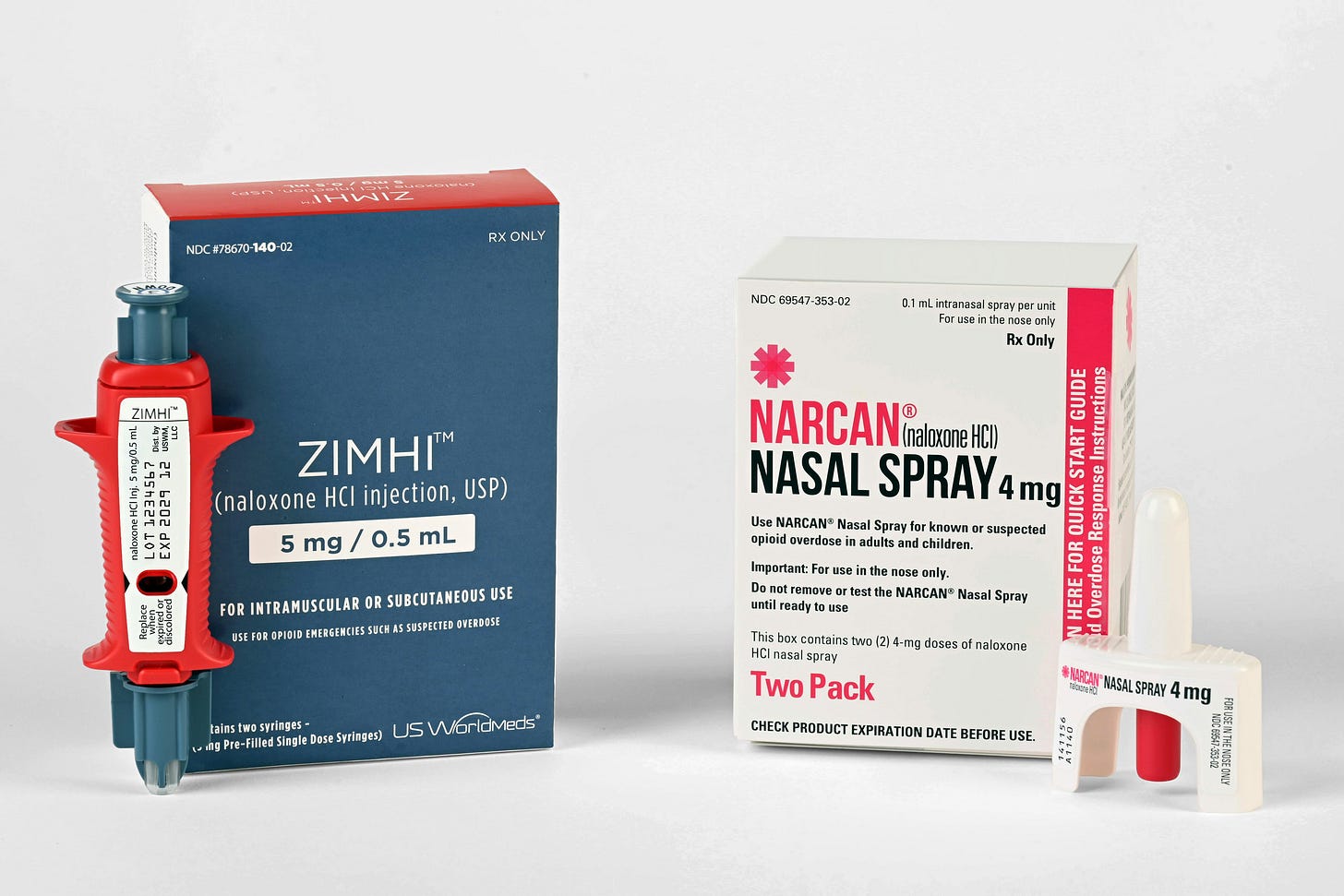
Naloxone, as in Beth’s case, is a lifesaver against opioid overdoses. Opioids are a type of medication commonly prescribed to relieve pain. They work by interacting with specific receptors in the brain and body to reduce pain perception. Examples include morphine, oxycodone, and codeine. Of course, opioids are also found in some illegal drugs, like heroin. While these medications can be effective for managing pain, they carry the risk of dependence and, in some cases, can lead to overdose.
Naloxone works by sticking to the same receptors in the body as opioids, blocking their effects, and quickly helping the person breathe normally again. This is crucial because opioids can slow down breathing to dangerous levels. Naloxone has no significant side-effects apart from the potential for acute opioid withdrawal. Only medical professionals used naloxone when it first came out in the 1960s. Soon after, however, it became weaponised for surveillance in the ‘war against drugs’ to help police identify and arrest people using opioids. Today, it is much more widely available in communities as a public health tool to save lives. Regular people like you and me can be trained to use it in a matter of minutes and can then carry it to help someone in an emergency. This shift recognises that anyone can play a role in saving lives. Although naloxone wears off and emergency medical intervention is always needed, this intervention can be the difference between life and death.

Blackpool, a seaside town in the north west of England where I serve as a Salvation Army officer, has been in crisis for a while. Despite a rich history, the town tops the league tables in England for many undesirable measures: lowest life expectancy for men and women; the highest rates of drug-related deaths; and the highest rates of hospital admissions for drug and alcohol related incidents. These challenges are often linked to underlying social issues such as poor quality housing, mental ill-health, and social isolation that are prevalent in areas of such deprivation. These issues are disproportionately affecting certain communities and people in the town, especially those experiencing homelessness, the criminal justice system, or those with a history of trauma.
While acknowledging the gravity of these issues, accurate measurement of drug use prevalence remains a challenge. Nonetheless, a 2016-17 study by Liverpool John Moores University revealed that Blackpool has an estimated 1,802 opiate users, representing a rate of 20.6 per 1,000 people. This positions the town as the second highest in England, trailing behind Middlesbrough in this unfortunate ranking. Addressing these complex, interrelated challenges requires a comprehensive and targeted approach, considering both the immediate issues and their underlying root causes. Equally, it is not a challenge that can be met by any individual organisation on its own.
The Salvation Army's historic emphasis in Blackpool has been on addressing rough sleeping, recognising it as the most visible layer of a complex metaphorical onion of interconnected ‘wicked issues.'1 As we peel back the layers, we uncover deeper-rooted causes such as mental health, domestic abuse, and, pertinent to our topic here, addiction. Further beneath these layers lie foundational issues of childhood trauma, relationship breakdown, and social dislocation, underscoring the depth of challenges faced by people in our community. Step by step, we have wanted to play a part in devising strategies that address not only the visible symptoms but also the underlying factors that shape the broader social issues.
The Salvation Army’s strategic power, however, is rooted in its practical wisdom, which we have needed to develop further on this issue. We saw the importance of working with partners to be able to respond. Our first step was to begin needle and syringe provision. The second was to inaugurate a service of commemoration for International Overdose Awareness Day. The third was to distribute naloxone to provide more opportunities to come into contact with people experiencing addiction to opioids. These initial approaches aim not only to respond to crises but also to establish relationships that can lead to more profound change.

In the ongoing effort to address opioid overdoses, the UK government is soliciting input on proposals to broaden access to naloxone without a prescription. Currently, only drug treatment facilities and healthcare professionals can supply naloxone. A new legal provision would make it much easier to get naloxone into the community and would allow churches like The Salvation Army, which also provide supported accommodation and outreach homelessness services, to be involved in that.
To get into the details of this, being able to distribute naloxone from The Salvation Army’s Bridge Project in Blackpool was a complex process. We needed to develop a tailored service level agreement (SLA) that aligns with the current regulations. This facilitates the distribution of naloxone by The Salvation Army in collaboration with the commissioned provider of drug and alcohol addiction treatment in Blackpool. This strategic legal instrument allows us to serve legally and faithfully in enhancing public health and safety. It covers things like the legal grounding, a partnership acknowledgement, geographical limitation, compliance assurance, and documentation and reporting.
We have a moral duty to do everything in our power to prevent people from dying of overdose. Furthermore, we recognise the transformative potential of addressing drug-related issues when people are in crisis. Many organisations would have similar convictions, but might not be able to navigate the current legal constraints. New legislation would make it easier for them to get naloxone into the community.
One of the nicknames for naloxone, the 'Lazarus Drug’ captures the dual impact of naloxone as a pharmaceutical tool in combating opioid overdose and a metaphorical link to the possibility of new life. The story of Lazarus in the Bible recounts how a close companion of Jesus is brought back to life after four days in the tomb. Naloxone, with its life-saving capabilities, embodies the contemporary pursuit to revive those teetering on the edge of death due to overdose. This prompts theological contemplation, urging churches to explore their potential pivotal role in addressing addiction and the challenge posed by opioid use.
Comparing the stories of Lazarus and Beth prompts reflection on compassion, intervention, and the emotions tied to averting a crisis. In both instances, the recognition of a body in distress prompts a compassionate response. Jesus’ deep response in his spirit manifests in his weeping, exemplifying the compassionate ethos of Salvation Army staff members supporting people going through addiction-related crises. While the response to Beth’s overdose necessitated more immediacy, both interventions exemplify a calm and purposeful approach.
Crucially, the commonality of resuscitation in both narratives underscores the transformative potential of timely and empathetic interventions. Much like Lazarus’ return from the dead, Beth's resuscitation symbolises a rebirth from the brink of mortality. The joy and relief that accompany averted crises resonate in both stories, highlighting the redemptive power inherent in compassionate responses. These parallels invite an appreciation of shared human experiences and the profound impact of extending care in moments of need. Just as Jesus did, so might we.
The paradigmatic character of ‘the addict’, however, also offers an avenue for encountering the presence of Christ within the context of vulnerability and crisis. Mirroring the biblical pattern of Matthew 25:31-46, the declaration “I was overdosed, and you gave me naloxone” provokes us to recognise Christ in moments of dire need. Just as Jesus identified himself with the hungry, the sick, and the imprisoned, the person facing addiction becomes a contemporary embodiment of Christ’s presence. The act of administering Naloxone becomes a tangible expression of compassion and care, even if the intervention is momentary and fleeting. It illustrates the potential for transformative encounters with the divine in the production of the possibility of ‘new life’ in the midst of a crisis moment. This perspective pushes us towards a theological exploration that extends beyond conventional boundaries, urging us to discern the sacred within narratives of addiction and recovery.

Thanks to the naloxone and the quick response of the staff team at Blackpool Salvation Army’s Bridge Project, Beth lived. Since being ‘brought back to life’ she has been able to make steps in other parts of her life, such as moving off the street into accommodation, and beginning to volunteer. Although naloxone itself is not what got her off the street, it kept her alive long enough to create the opportunity for her to make the change she wanted to. Essential to this has been the wider community of people in recovery, and supportive friends who are interested in Beth for the long haul.
There could have been a disastrous outcome for Beth.
Thank God that isn’t what happened.
Thank God for evidence-based measures to reduce drug-related deaths.
Thank God for Naloxone and the staff.
May we act on every opportunity “to keep people alive until we can actually build a system that can help people with substance use, addiction, and mental health.”2
May we deepen our understanding of people so that, rather than merely “trying to change the behaviours of addicted human beings,” we focus on “healing the pain that drives those behaviours.”3
May we experience such compassion that, like Jesus, we might be able to save friends from early death.
Wicked Issues are “.. difficult or impossible to solve because of incomplete, contradictory, and changing requirements…not resolved by traditional “technical” managerial approaches to the provision of public services”, Rittel and Webber, 1973.
Maté, Gabor. In the Realm of Hungry Ghosts.
Ibid.



Great article John. You are absolutely right- Naloxone saves lives and creates an opportunity for people to find a new life. In the states they have nasal spray Naloxone in vending machines. Addiction is a public health issue- not a criminal justice issue and it’s great to see that we are providing a medical intervention. Well done to Jill and the team at the Bridge